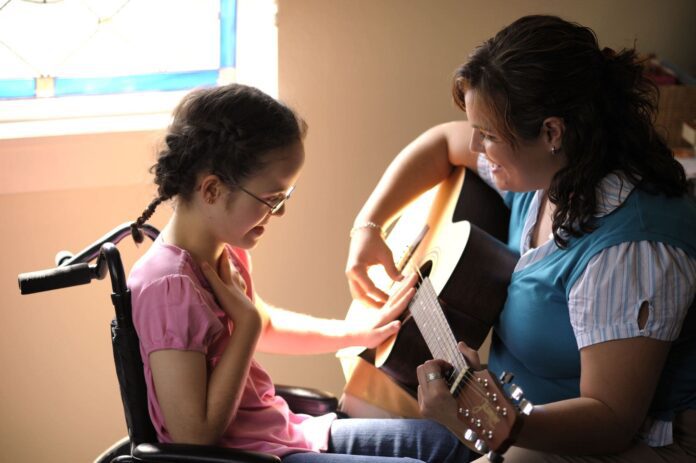“I have a passion for music,” declares 52-year-old April Mobley of Cocoa Beach. So when her nurse, Katherine, mentioned the concept of music therapy, Mobley, who especially loves acoustic guitar, felt amped up! “Everything in my life revolves around music,” she says.
Mobley is receiving treatment for both leukemia and diabetes at Florida Hospital Orlando. Due to complications with diabetes, she recently lost a toe and is struggling with her emotions about her health. But music therapy cheers her up.
“I’m happy when she [the therapist] is here. When she plays the guitar, I forget about all my problems,” she says. Mobley’s positive response to music therapy is shared by other patients.
How Music Therapy Heals
“One of the things that I love about music therapy is that we’re able to individualize it to the person. So, the benefits – anecdotally and according to research – are quite wide-ranging. It can really encompass the whole person because there are physical benefits, and physiological, neurological, social and spiritual,” says Rich Abante Moats, a board-certified music therapist who serves as the Music Therapy Program Manager at Florida Hospital. In 2017 alone, Florida Hospital led 8,000 music therapy sessions ─ a collaborative sum of independent and group meetings.
Music therapy, as defined by the American Music Therapy Association, “is the clinical and evidence-based use of music interventions to accomplish individualized goals within a therapeutic relationship by a credentialed professional.” The concept has struck a chord within the field of medicine and is benefiting patients with diverse conditions, such as anxiety, autism, asthma, chronic pain, dementia, depression, end of life care, irregular sleep patterns, mobility issues, Parkinson’s disease, stroke and traumatic brain injury.
After evaluating the strengths and needs of an individual, music therapists guide therapeutic treatments that may include playing instruments, songwriting, singing and moving to and/or listening to music. Music therapists must earn a music therapy degree, complete a minimum of 1,200 hours of clinical training and pass a certification exam. Moats says those unfamiliar with the specialty question how music therapy differs from someone just turning on the radio.
“A music therapist has the ability to assess and to change how music is presented according to the person’s ability. It is always success-oriented,” she says. “A radio can’t change the tempo. We can make adjustments so the brain won’t be overstimulated.”

Photo: David Akins enjoys music therapy at Florida Hospital.
For example, when working with stroke patients, Moats aims to improve communication, mobility and cognitive function. “I may use singing to emulate a phrase the patient is working on. We train the patient to sing a phrase and work on rhythms,” she describes.
This approach of layering words on top of melody and rhythm was also embraced by Congresswoman Gabby Giffords. She experienced aphasia ─ the inability to speak ─ following a brain injury from a gunshot. Additionally, to foster muscle control with stroke or brain injury patients, Moats says, “If we’re doing shoulder flexion, a patient may use a mallet with drums and we have a metronome that keeps us in time.”
Music therapy, as defined by the American Music Therapy Association,“is the clinical and evidence-based use of music interventions to accomplish individualized goals within a therapeutic relationship by a credentialed professional.”
Erin Keenan, a music therapist who researched Parkinson’s disease at the University of Miami, says music can help with side effects associated with the disease, such as shuffling gait, tremors, muscle rigidity and speech change. During an interview with The Miami Hurricane, she shared, “Music gives the central nervous system so much information. There is so much going on in the brain, and rhythm helps organize everything.”
Marty Miller agrees. Her husband, David Akins, is losing his voice as a result of his fifteen-year battle with Parkinson’s. Miller says music therapy has helped him to speak louder. “As a caregiver, you have to try it with your loved ones so you can encourage them when they feel like stopping. It’s up to us to keep them moving,” she attests, adding, “We get in the car and we start to practice, so we go ‘la, la, la’ when no one can hear us sing.”
Akins also appreciates the support of his fellow patients. “Besides the positive impact it has had on my health, I do it because it allows me to socialize with other people. The other participants are my family ─ an extended family that’s always there for me when I need them. I’m friends with each and every one of them,” he says.
Moats and her small team of seven help patients battling cancer to work on emotional goals and coping mechanisms as well. “We may focus on verbal discourse and talk about feelings and their journey; then, write about those feelings and transform them into a song.” And Moats also witnesses progress within the neonatal intensive care unit (NICU). She’s not exactly looking to mold mini Beethovens, per se, but rather implement scientific findings. Researchers at the Louis Armstrong Center for Music and Medicine at Beth Israel Medical Center in New York found that infants who had respiratory distress or sepsis tended to do better while listening to sounds mimicking a heartbeat, fluid in the womb or lullabies.
Music Therapy for Youthful Players
Music therapy is actually implemented in many settings beyond hospitals. Joyful Music Therapy in Orlando, for example, offers individual and group music therapy, adaptive lessons and other sessions. The company focuses on individuals with autism, early intervention, memory care, geriatrics and hospice. “We provide therapeutic music instruction to many children and adults with special needs. As music therapists, we are trained to focus on the strengths of the individual so our music lessons are far from traditional. However, our students perform in bi-annual recitals,” says Tamela Ponder, a board-certified music therapist and Executive Director/Founder of Joyful Music Therapy.
Jennifer Sikora credits Joyful Music Therapy with empowering her son, Sean, who has Down syndrome, to not only increase his knowledge of music but also gain confidence and improve communication and expression skills. “Integrating music with movement and a routine helped him to become more confident, the sharing of musical instruments helped him to learn to take turns and communicate with his peers, and the various listening games helped him to learn to be an active listener,” Sikora explained. Sikora and other parents have lobbied in support of the Florida Music Therapy Government Relations Task Force to create a music therapy registry (SB 562/HB 729).
Furthermore, while it’s not technically a music therapy service, fine arts community groups (like Orlando Philharmonic Orchestra) host sensory-friendly concerts to welcome audience members of all abilities to experience musical performances in a comfortable environment.
Photos courtesy of Florida Hospital and Joyful Music Therapy